The human eye is often compared to a traditional film camera. While the lens at the front focuses light, the retina at the back acts as the film, capturing images and sending them to the brain. When a patient develops a cataract – a clouding of the natural lens – the “viewfinder” becomes blurry. However, for patients with underlying retinal diseases like macular degeneration or diabetic retinopathy, cataract removal is not a simple “plug-and-play” procedure. It requires a sophisticated, multidisciplinary approach to ensure that clearing the lens doesn’t inadvertently damage the fragile “film” at the back of the eye.
Cataract Treatment and Pre-Surgery Prep: Stabilizing the Retina
Before a surgeon even considers cataract removal surgery, the priority is the health of the posterior segment. In patients with retinal pathologies, the inflammatory response triggered by surgery can exacerbate existing conditions. Therefore, eye cataract treatment begins weeks, sometimes months, before the actual procedure.
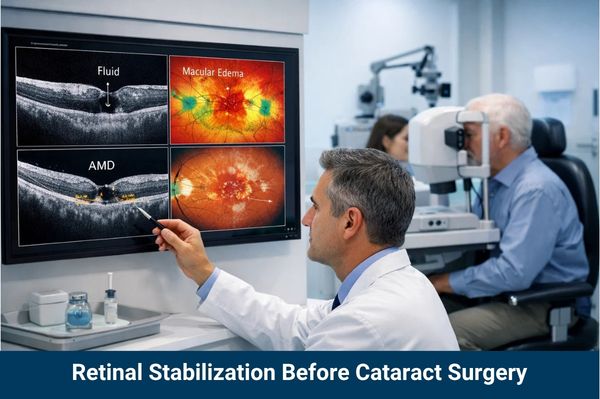
Stabilization typically involves high-definition imaging known as Optical Coherence Tomography (OCT). This allows doctors to look for “wet” markers in Age-Related Macular Degeneration (AMD) or swelling in Diabetic Macular Edema (DME). If the retina is “leaking,” the surgeon may administer anti-VEGF injections or perform laser treatment for cataract preparation to stabilize blood vessels. A stable retina is the foundation of a successful surgical outcome; proceeding on an unstable retina is like painting a masterpiece on a crumbling wall.
Read Our Article
How to Delay Cataract Surgery: 7 Proven Lifestyle ShiftsCataract Surgery: Utilizing Gentler Surgical Methods
Standard cataract surgery usually employs a technique called phacoemulsification, where ultrasound energy breaks the cloudy lens into tiny pieces. While efficient, this energy creates “turbulence” inside the eye that can be taxing on a sensitive retina. For these high-risk patients, surgeons often pivot to “soft-shell” techniques.
These gentler methods involve using highly viscous fluids to protect the eye’s internal structures and employing “low-energy” or “slow-motion” phacoemulsification. By reducing the total amount of energy dispersed inside the eye, the surgeon minimizes the risk of a “sympathetic” inflammatory response in the retina. This careful modulation of fluidics and energy is what separates a routine cataract eye surgery from a specialized retinal-care procedure.
Toric Lenses for Cataract Surgery and Choosing the Right Replacement
When patients research cataract surgery cost, they often encounter various “premium” lens options. For a healthy eye, multifocal or “all-in-one” lenses are popular because they reduce the need for glasses. However, for patients with retinal disease, these lenses can be counterproductive. Multifocal lenses split light into different focal points, which inherently reduces “contrast sensitivity” – the ability to distinguish an object from its background.
Since retinal diseases already diminish contrast, most specialists recommend high-quality monofocal lenses. These lenses focus all light onto a single point, providing the crispest possible image to a compromised retina. If the patient has astigmatism, toric lenses for cataract surgery are often the gold standard. They correct the irregular shape of the cornea without the visual “noise” of multifocal optics, ensuring that the damaged retina receives the highest quality signal possible.
Testimonials
“Excellent manner, listens really well and gives multiple opportunities to ask questions, which is really helpful. Very calm, gently spoken and not rushed”
Cataract Eye Surgery: The "Two-in-One" Combined Procedure
In certain advanced cases, a patient might suffer from both a dense cataract and a surgical retinal issue, such as a macular hole or an epiretinal membrane. In these instances, the medical team must decide between staged surgeries or a combined “phaco-vitrectomy.”
The Pros of Combined Surgery:
- Efficiency:One trip to the operating room and one recovery period.
- Visibility:Removing the cataract gives the retinal surgeon a crystal-clear view of the back of the eye, allowing for more precise retinal repair.
The Cons of Combined Surgery:
- Complexity:Longer operative times can increase the risk of post-operative pressure spikes.
- Refractive Shifts:It is harder to predict the final vision outcome when the eye is undergoing two major structural changes simultaneously.
Our Other Treatments
Corneal Collagen Crosslinking (CXL) Eye SurgeryLaser Eye Surgery for Cataracts: Managing Swelling and Recovery
The single greatest threat to vision after cataract removal surgery in this patient population is Cystoid Macular Edema (CME) – swelling in the central part of the retina. To prevent this, the recovery protocol is much more aggressive than standard cases.
While a typical patient might use drops for two weeks, a retinal patient might remain on potent anti-inflammatory drops for months. In some cases, surgeons use laser eye surgery for cataracts to ensure precise incisions that heal faster or they may even inject slow-release steroid implants into the eye during surgery. These “internal shields” provide a steady dose of medication directly to the retina, fighting inflammation from the inside out during the critical first 30 days of healing.
Laser Treatment for Cataract: Navigating Past Eye Surgeries
Patients who have previously undergone a vitrectomy (removal of the eye’s internal gel) present a unique challenge during cataract treatment. Without the natural support of the vitreous gel, the lens can become “bouncy” during surgery, making it harder for the surgeon to stabilize.
Furthermore, if the patient has had laser treatment for cataract complications or retinal tears in the past, there may be scar tissue or “zonular weakness” (the tiny fibers holding the lens in place). Surgeons must navigate these “pre-operated” eyes with extreme caution, often using specialized rings to manually expand the pupil or support the lens capsule, ensuring the new IOL stays perfectly centered.
Cataract Removal: Managing Expectations and Visual Outcomes
Perhaps the most important part of cataract surgery for retinal patients is the “pre-op talk.” It is essential to manage expectations regarding what the patient will actually see. If a patient has advanced Macular Degeneration, removing a cataract will clear the “fog” and improve peripheral vision, but it cannot restore the central “blind spot” caused by the retina.
Doctors use the “ceiling of potential” analogy: if the retina is only capable of 20/60 vision, the best cataract eye surgery in the world cannot bring them to 20/20. However, for many, the jump from “legal blindness” to being able to navigate their home or see large print is a life-changing outcome that makes the procedure well worth the effort.
Conclusion: A Clearer Path Forward
In the modern era of ophthalmology, having a retinal disease is no longer a barrier to receiving high-quality cataract treatment. Through the use of advanced diagnostics, “low-energy” surgical techniques and specialized toric lenses for cataract surgery, surgeons can safely navigate the complexities of a compromised eye. While the journey requires more preparation and a longer recovery, the result – restored clarity and improved quality of life – remains one of the greatest triumphs of modern laser eye surgery for cataracts. By prioritizing retinal stability and setting realistic goals, patients can once again see the world with newfound brightness.
