The landscape of ophthalmology has been fundamentally altered by the advent of high-resolution imaging, specifically Optical Coherence Tomography (OCT). Once used primarily as a diagnostic tool for retinal diseases, OCT has now become a cornerstone of cataract treatment and surgical planning. By utilizing light waves to capture cross-sectional, micron-level images of the eye’s internal structures, this technology allows surgeons to visualize the eye in ways that traditional microscopes cannot.
Modern cataract surgery has shifted from a basic restorative procedure to a precision refractive surgery. Patients now expect not only the removal of their cloudy lens but also a significant reduction in their dependence on glasses. To meet these high expectations, surgeons must account for every anatomical variable. This article explores how OCT technology ensures that eye cataract treatment is personalized, safe and highly accurate.
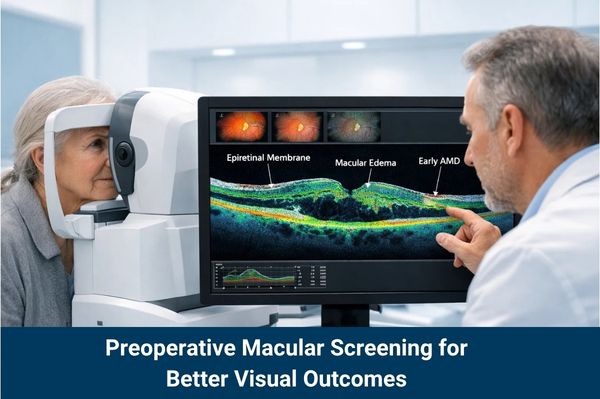
Preoperative Macular Screening for Optimized Visual Outcomes
The most critical factor in the success of cataract removal surgery is the health of the retina. A cataract acts like a dirty window; while the window can be replaced, the “view” will remain poor if the camera’s film – the macula – is damaged. OCT provides a detailed “optical biopsy” of the macular layers, detecting pathologies that are often invisible during a standard clinical exam.
Common conditions such as Epiretinal Membranes (ERM), Macular Edema or early-stage Age-Related Macular Degeneration (AMD) can significantly limit the vision a patient gains after cataract removal. By identifying these issues beforehand, the surgeon can adjust the surgical plan, manage patient expectations and determine if the patient is a suitable candidate for premium lens options.
Precise Biometry and IOL Power Calculations Through Advanced Scans
Achieving “20/20” vision after cataract surgery depends on choosing an Intraocular Lens (IOL) with the perfect power. Modern OCT-based biometers have replaced older ultrasound methods because they provide non-contact, ultra-accurate measurements of the eye’s axial length and corneal curvature.
The precision of OCT-based biometry allows surgeons to use the latest generation of IOL calculation formulas. This ensures the lens power is spot-on, which is essential for patients who wish to avoid wearing glasses for distance or reading. This data-driven approach is a primary reason why the success rates of cataract eye surgery have reached all-time highs.
Management of Post-Refractive Surgery Eyes and TCRP
Patients who have previously undergone laser eye surgery for cataracts or refractive procedures like LASIK and PRK present a unique challenge. Their corneas have been reshaped, making standard lens power formulas inaccurate. This is often where “refractive surprises” occur, leading to blurry vision after surgery.
OCT solves this by measuring the Total Corneal Refractive Power (TCRP). Instead of assuming the relationship between the front and back of the cornea, OCT measures both surfaces directly. This allows the surgeon to account for the true refractive power of the eye, ensuring that the cataract surgery cost results in the clear vision the patient deserves, regardless of their surgical history.
Testimonials
“Extremely gentle, professional and informative, Could not wish for more”
Detection of "Occult" Glaucoma and RNFL Analysis
Cataracts often develop in the same age group most at risk for glaucoma. Unfortunately, a dense cataract can obscure the surgeon’s view of the optic nerve during a routine check. OCT allows for a precise analysis of the Retinal Nerve Fiber Layer (RNFL) thickness, even through a cloudy lens.
If “occult” or hidden glaucoma is detected early, the surgeon can provide a more comprehensive cataract treatment. In many cases, a Micro-Invasive Glaucoma Surgery (MIGS) device can be implanted during the same cataract removal procedure. This dual-purpose approach manages eye pressure and restores clarity in a single surgical session.
Intraoperative OCT (iOCT) for Real-Time Surgical Precision
One of the most significant leaps in laser treatment for cataract and manual surgery is Intraoperative OCT (iOCT). This technology integrates the OCT scanner directly into the surgeon’s operating microscope. This allows for a “heads-up” cross-sectional view of the eye’s structures in real-time during the surgery.
For the surgeon, this provides an extra layer of safety during difficult steps, such as confirming the depth of a corneal incision or ensuring the replacement lens is seated perfectly within the capsular bag. iOCT is particularly helpful in complex cataract removal surgery where traditional 2D visualization may not provide enough depth information.
Our Other Treatments
Corneal Collagen Crosslinking (CXL) Eye SurgeryAssessing Corneal Ectasia and Irregularity for Premium Lenses
The use of toric lenses for cataract surgery or multifocal IOLs requires a very regular and healthy corneal surface. If the cornea has subclinical keratoconus (thinning) or significant irregularity, these “premium” lenses will not function correctly, potentially causing glare or halos.
OCT-based epithelial mapping is used to identify these subtle corneal irregularities. By mapping the thickness of the epithelium across the eye, the surgeon can confirm if the patient is a candidate for high-tech lenses. This preoperative screening is vital for ensuring that laser eye surgery for cataracts meets the high visual demands of the modern patient.
Postoperative Complication Monitoring and Cystoid Macular Edema
The role of OCT does not end when the surgery is over. If a patient experiences a “blur” after a technically perfect cataract eye surgery, OCT is the first diagnostic tool used to investigate. It is the gold standard for detecting Cystoid Macular Edema (CME), a common form of inflammatory swelling that can occur after surgery.
Because OCT can detect fluid at a microscopic level, surgeons can begin treatment with medicated drops immediately. It is also used to check the tilt or centration of the new lens, ensuring that any mechanical issues are identified and corrected during the early recovery phase of eye cataract treatment.
Conclusion
Optical Coherence Tomography has revolutionized the way surgeons approach cataract treatment. By providing a transparent view of the eye’s internal health – from the cornea to the retina – OCT has removed the guesswork from surgical planning. Whether it is ensuring the accuracy of toric lenses for cataract surgery or detecting hidden glaucoma, this technology provides the data necessary for a successful outcome. As digital technology continues to advance, OCT remains the most vital tool in transforming cataract removal into a life-changing refractive experience.
